In the realm of medical innovation, diabetic limb preservation surgery shines as a beacon of hope. Consider Michael, who feared amputation due to his severe diabetic complications, but saw new possibilities after surgery restored his mobility.
There is hope.
Thousands now find relief through these surgical advancements, transforming potential despair into vibrant new chapters of life, replete with promise and renewed independence.
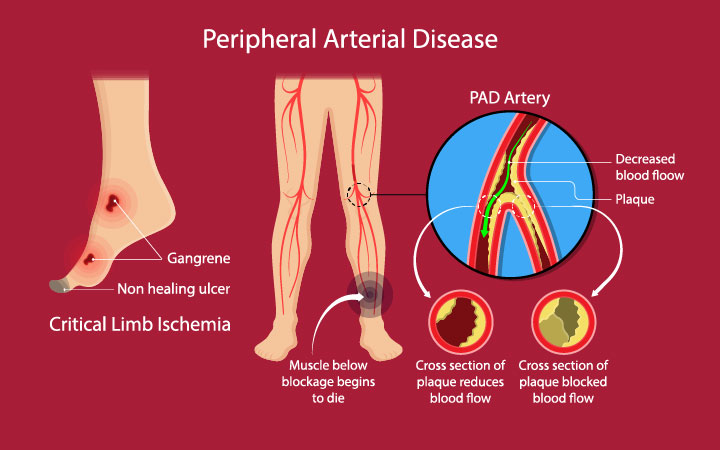
Understanding Diabetic Limb Preservation Surgery
At its core, diabetic limb preservation surgery aims to prevent the progression to amputation.
This surgery is a sophisticated fusion of medical science and compassionate care, specifically tailored for individuals with diabetes. These individuals often face challenges with their lower extremities due to compromised circulation and neuropathy. By focusing on restoring blood flow and addressing infection threats, surgeons work diligently to save the limb and significantly enhance the patient’s quality of life.
Through meticulous surgical techniques, circulation is improved, allowing tissues to recover. This involves removing any dead tissue, followed by cutting-edge procedures to increase blood flow, thereby facilitating natural healing and reducing future risks. Our Seattle office is experienced in caring for diabetic foot complications and initiating necessary referrals for vascular surgery.
Ultimately, the surgery not only strives to preserve physical function but also empowers patients with a renewed sense of independence and possibility. It represents a symbol of resilience, demonstrating that with innovation and expertise, we can challenge the status quo and provide life-affirming outcomes for those affected by diabetes, transforming daunting prognoses into triumphant recoveries.
Identifying the Need for Surgery
Recognizing signs of deterioration is crucial.
Early indicators such as persistent foot ulcers, diminished circulation, and repeated infections can herald the need for diabetic limb preservation surgery. Such symptoms must not be taken lightly, as they can escalate quickly, inflicting irreversible damage. Physicians like Dr. Hoy, guided by a keen sense of urgency, prioritize identifying these early-warning signals to safeguard the patient’s future well-being.
A prompt diagnosis can save a limb.
Through regular monitoring, healthcare professionals can discern the appropriate moment to intervene surgically. This timely decision significantly enhances the potential for success, underpinning the hope of restoration and healing.
With the aid of advanced diagnostics and cutting-edge imaging techniques, physicians can now evaluate the intricate complexities of each patient’s condition. This ensures that the path to surgery is embarked upon with clarity and precision, bolstering confidence in a prognosis of success.
Factors Leading to Amputation Risks
Diabetes can significantly elevate the risk of amputation through various interconnected factors. Chief among these are neuropathy, poor circulation, and susceptibility to infection, which are often heightened as the disease progresses.
Neuropathy reduces pain sensation, delaying detection of injuries.
Such conditions create a precarious landscape for wound healing, as even a minor injury can evolve into a severe complication in the presence of inadequate blood flow and heightened infection risk. This trifecta, driven by diabetes, underscores the critical need for vigilance, proactive care, and timely intervention.
Moreover, lifestyle choices contribute to the sheer scale of risk, with smoking and obesity serving as amplifiers of vascular issues and nerve damage associated with diabetes. By understanding these complex contributing factors, a robust prevention and intervention strategy can be developed, emphasizing personalized care. This proactive approach, underpinned by “prevention,” is essential to effectively manage and reduce these risks.
Key Benefits of Limb Preservation
Limb preservation is a transformative approach for individuals.
The procedure’s primary benefit lies in maintaining the function and quality of life. By saving the limb, patients can better retain their mobility, independence, and overall well-being. Moreover, it alleviates the psychological burden associated with amputation, fostering a sense of hope and resilience.
Retaining limbs leads to improved patient outcomes.
Advancements in diabetic limb preservation surgery ensure that patients experience a significantly enhanced quality of life – not only because they retain autonomy in daily activities – but also through reduced rehabilitation time and improved mental well-being.
These surgical interventions in diabetic limb preservation surgery represent groundbreaking innovations in medical practice, empowering many to overcome challenges. With the advent of new technologies and techniques, these procedures have the potential to redefine patient experiences, enhancing recovery and establishing a new paradigm for proactive, life-affirming healthcare.
Preparing for Surgery
Preparing for diabetic limb preservation surgery requires a blend of strategic medical planning, teamwork, and personal resolve. Embracing this opportunity begins with comprehensive consultations, ensuring all aspects are understood and managed, paving the way for a successful surgery that upholds one’s quality of life and longevity.
Pre-Surgery Consultation
Before embarking on diabetic limb preservation surgery, compassionate and comprehensive consultations are essential to prepare patients both mentally and physically for the journey ahead.
Proper preparation can reduce post-surgery complications, owning this responsibility ensures optimal outcomes and fosters recovery.
During these consultations, the interdisciplinary medical team assesses the patient’s overall health, discusses the surgical approach, and sets realistic expectations. This holistic review is crucial for identifying and minimizing potential risks.
Together with cutting-edge technology, a collaborative spirit infuses the pre-surgery process—transforming individual patient needs into a personalized roadmap for success, thus building trust and confidence in the medical journey.
Risk Assessment and Management
Effective risk assessment is pivotal in diabetic limb preservation surgery. It ensures patient safety and enhances surgical outcomes, offering a life-changing opportunity.
- Comprehensive Medical Evaluation: Identifies pre-existing conditions and potential complications.
- Interdisciplinary Collaboration: Facilitates a thorough understanding of patient needs.
- Customized Treatment Plans: Tailored to unique patient risk factors.
- Continuous Monitoring: Enables real-time adjustments and proactive management.
These components collectively form a robust foundation for successful limb preservation. Addressing risks early enhances patient confidence and recovery.
Incorporating cutting-edge technologies further refines the risk management process, transforming potential challenges into triumphs of surgical precision.
Surgical Techniques in Focus
In the realm of diabetic limb preservation surgery, surgical techniques have evolved into powerful tools of hope and healing, marked by remarkable advancements in precision and efficacy.
Advanced technologies have paved the way for innovative approaches in surgical interventions. These developments enhance the accuracy and outcomes of procedures.
For instance, minimally invasive techniques such as endovascular surgery offer targeted solutions by utilizing state-of-the-art imaging technologies.
These techniques aim to improve blood flow, thereby significantly reducing the risk of amputations and enhancing the healing process for diabetic patients.
The integration of micro-surgical expertise and robotic-assisted procedures exemplifies a new era of surgical excellence, showcasing the pinnacle of precision and patient-centered care. This ensures superior outcomes in limb preservation.
Undoubtedly, the focus on innovation in surgical techniques drastically elevates the standard of care. It fuels optimism in both patients and medical practitioners alike, reinforcing a shared vision of healthier living.
Post-Surgery Care and Recovery
Post-surgery care is an essential phase, ensuring a smooth recovery and optimal outcomes following diabetic limb preservation surgery. Adhering to a well-structured recovery plan supports long-term success.
Rest and proper wound care are at the forefront, laying a foundation for effective healing.
Typically, patients should monitor for signs of infection, swelling, or discoloration, thereby preventing complications.
Physical therapy plays an instrumental role in rebuilding strength and flexibility, promoting a swift return to normal activities.
A multidisciplinary approach, incorporating regular consultations with a healthcare team, empowers patients to actively participate in their recovery journey, fostering resilience and adaptive strategies.
Ultimately, every step of one’s recovery process is guided with care. Thoughtfully designed post-operative care plans provide the crucial support necessary to ensure enduring well-being, reflecting a brighter and healthier future.
Monitoring and Follow-up Visits
Essential for sustained recovery progress.
Consistent follow-up visits play a pivotal role in the rehabilitation process. These visits are designed to assess the patient’s recovery and address any emerging issues promptly, ensuring that healing occurs as expected. Moreover, they provide an avenue for personalized guidance, reinforcing the confidence patients need to manage their condition successfully.
The frequency of monitoring can vary.
Regular assessments include checking vital signs – not only for wound healing but for broader systemic health – as part of diabetes management can often unveil other health anomalies. It underscores the holistic benefit of post-surgical monitoring.
Engaging in follow-up visits fosters proactive communication, enabling healthcare professionals to address queries, update treatment protocols, and adjust lifestyle recommendations as needed. This collaborative approach, buoyed by advancements, ensures that patient care remains at the forefront. Such visits foster a sense of partnership and commitment, aligning medical insights with the patient’s personal health goals, solidifying the path to recovery.
Potential Complications and Their Management
Diabetic limb preservation surgery, like any medical procedure, carries the potential for complications that can impact recovery and outcomes.
These risks, however, are often mitigated by a comprehensive preoperative assessment and meticulous surgical technique, securing optimal results. Possible complications could include infection, impaired wound healing, or vascular issues. Early identification and intervention prove indispensable, with innovations in wound care and vascular therapy playing crucial roles in managing these challenges.
For instance, infections may necessitate a multifaceted approach to stop progression. In practice, this often involves antibiotics, tailored wound care regimens, and sometimes further surgical intervention to ensure the continuation of healing while preserving maximum limb function and health.
Ultimately, addressing potential complications requires a proactive strategy rooted in vigilance and advanced medical practices. Coordinated care from a multidisciplinary team can substantially decrease risks, utilizing state-of-the-art diagnostics and therapeutics that transform challenges into opportunities. Patient education alongside expert intervention helps to empower individuals, creating an affirmative pathway to resilient recovery and improved quality of life.
Role of a Multidisciplinary Team
A multidisciplinary team unites diverse expertise for optimal diabetic limb preservation surgery outcomes. Through collaboration, these experts enhance recovery and quality of life.
Such teams often involve vascular surgeons, endocrinologists, podiatric foot and ankle surgeons, wound care specialists, and nutritionists. Each brings a unique perspective.
By integrating their specialized skills, team members identify and address complex challenges. This comprehensive approach ensures a seamless continuum of care, maximizing the potential for successful limb preservation.
The strength of a multidisciplinary team lies in its ability to offer a holistic plan tailored to individual patient needs. To strengthen patient outcomes, it’s vital to blend clinical insights and cutting-edge innovations, nurturing a culture of shared success, hope, and remarkable clinical triumph.
Patient Education and Support Systems
Patient education serves as a cornerstone of diabetic limb preservation surgery, offering patients a robust understanding of their condition, inspiring a motivational paradigm shift across their life.
Comprehensive education programs provide insights into effective self-management strategies.
With knowledge, patients can make informed decisions regarding care protocols (including lifestyle adaptations), leading to empowered wellness.
Support systems should include diverse patient-centered interventions to optimize limb preservation, facilitating proactive healthcare decisions.
These programs include personalized education sessions to address unique patient concerns, encouraging the pursuit of optimal outcomes by creating individualized care plans and fostering active patient engagement.
Ultimately, the goal is to ensure that every patient’s journey is one of empowerment and efficiency. Continued educational efforts coupled with supportive environments reinforce a patient’s resilience amid their healthcare journey.
Lifestyle Changes for Better Outcomes
Embracing lifestyle changes is paramount for enhancing the success of diabetic limb preservation surgery. By adopting healthier habits, patients not only improve their surgical outcomes but also enrich their overall well-being.
Regular physical activity significantly boosts circulation, aiding in wound healing. Additionally, it is essential for maintaining optimal blood sugar levels.
Nutrition plays a critical role, and a balanced diet rich in vitamins and minerals propels patients towards a journey of sustained health. Diets focusing on whole foods, lean proteins, and minimal sugars provide robust support to surgical outcomes.
Such lifestyle modifications empower individuals to take charge of their health journey, creating a continuum of care beyond surgery, making them active participants in their recovery and long-term wellness. Hence, focusing not merely on “survival” but on thriving with renewed vigor and vitality.
Advances in Diabetic Limb Preservation Surgery
Remarkable strides are transforming diabetic limb preservation.
Cutting-edge technologies have brought new hope to those affected. The latest advances not only enhance the intricate procedures of diabetic limb preservation surgery but also significantly reduce recovery time and improve outcomes. Today, innovations in the art of surgery are building upon decades of dedicated research to save more limbs and transform countless lives.
Advanced imaging significantly enhances surgical precision.
New surgical techniques are propelled by – and indeed some might say emerge because of – these advancements, with surgeons employing state-of-the-art, minimally invasive procedures that redefine success rates.
These profound innovations in diabetic limb preservation surgery unlock exceptional possibilities for the future. Utilizing the latest scientific insights alongside expert surgical techniques, patients are witnessing highly successful outcomes that bring hope and healing. These changes empower individuals with diabetes, affirming their journey toward renewed life quality and reinforcing our collective commitment to advancing patient care.
Real-Life Success Stories and Testimonials
Amazing transformations inspire many in this journey.
One patient, Courtney, found new hope and vitality. Her journey epitomizes the miraculous potential of diabetic limb preservation surgery, leading to an active lifestyle void of prior limitations. Encouraged, she now dedicates her time to advocating for people facing similar challenges by sharing her story.
Michael is resilient, overcoming the odds.
Through skilled surgical intervention and post-operative care – all which would have once seemed impossible to achieve – he has regained cherished mobility, returning to long walks and familial adventures he greatly values.
Countless patients continue to share similar exhilarating experiences, profoundly inspiring healthcare professionals who see the palpable impact of their dedication. Reflecting on the positive outcomes witnessed thus far, there’s an invigorating momentum. There emerges a powerful narrative of reclaiming life, endeavoring toward limitless potential unbounded by past constraints.
