Foot osteomyelitis is a serious infection of the bone in the foot, most commonly caused by bacteria. It can result from an open wound, a foot ulcer, or spread from nearby tissue. If left untreated, foot osteomyelitis can lead to chronic pain, bone damage, or even amputation.
This condition is particularly common in individuals with diabetes, poor circulation, or compromised immune systems.
When bones in the foot become infected, it affects everything from a person’s ability to walk to their general sense of well-being. Foot osteomyelitis, while less discussed than other forms of infection, can have a major influence on daily life, especially for those at higher risk. Unlike minor injuries or even some other infections, this condition involves bone tissue itself becoming infiltrated by bacteria or, less commonly, fungi.
Osteomyelitis is not a new diagnosis. Medical writings as far back as the 19th century described “caries of the bone,” now recognized as this painful and sometimes stubborn infection. Today, advanced imaging and modern antibiotics have improved outcomes, but the condition remains challenging, particularly when it occurs in the foot.
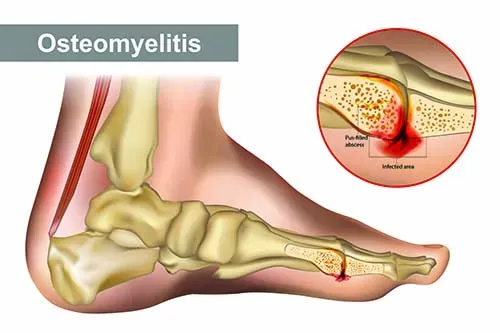
What is Foot Osteomyelitis?
Foot osteomyelitis refers to an infection in the bones of the foot, most often caused by bacteria entering through a wound, surgery, or the bloodstream. The bones commonly affected include the metatarsals, tarsal bones, or the calcaneus (heel bone). This infection can progress rapidly or develop slowly over weeks, quietly damaging bone and surrounding tissue.
Foot infections stand out among osteomyelitis cases because the unique structure of the foot, with its many small bones and limited soft tissue coverage, can make treatment especially difficult. Complicating factors, such as poor circulation or diabetes, often play a role in both the development and persistence of infection.
How Does the Infection Start?
Understanding how infection finds its way into bone tissue is key. The three primary routes are:
- Direct Inoculation: Common in cases of open fractures, wounds that expose the bone, surgical procedures, or penetrating injuries such as stepping on a nail. The bacteria bypass the skin and soft tissues and reach bone almost immediately.
- Contiguous Spread: This happens when a bone infection starts from an adjacent tissue that is already infected, such as an ulcer or cellulitis. Diabetic foot ulcers are a frequent culprit here.
- Hematogenous Spread: In this scenario, bacteria travel through the bloodstream from another site of infection, lodging in the bone. While more common in children, it can happen in adults with compromised immune systems.
In people without diabetes or immune problems, bones usually resist infection well. The presence of chronic wounds and reduced blood flow, seen especially in diabetic neuropathy and peripheral artery disease, lowers the body’s ability to fight off these invaders.
Who is At Risk?
While foot osteomyelitis can affect anyone, certain groups face a higher likelihood of developing this infection. Major risk factors include:
- Diabetes mellitus, particularly with poorly controlled blood sugar and neuropathy, especially with diabetic foot ulcers
- Peripheral arterial disease (poor blood supply to the legs and feet)
- Chronic foot ulcers or wounds, especially those lasting more than a few weeks
- Immune suppressive conditions, such as HIV/AIDS, chronic steroid use, or chemotherapy
- Recent foot surgery or trauma
- IV drug use
- Alcoholism and associated liver disease
A closer look at one of these, diabetes, shows why the foot is particularly vulnerable to infection. Damage to nerves blunts pain perception, so injuries may go unnoticed. Poor circulation means that both immune cells and antibiotics have a difficult time reaching the site. This sets the stage for bacteria to take hold, often in places where the skin has broken down or blisters have formed.
What Causes Foot Osteomyelitis?
The overwhelming majority of cases involve bacteria. The table below provides a snapshot of the most common pathogens:
| Pathogen | Typical Source |
|---|---|
| Staphylococcus aureus | Puncture wounds, ulcers, bloodstream |
| Streptococcus species | Wounds, especially in diabetics |
| Pseudomonas aeruginosa | Moist environments, puncture wounds through shoes |
| Enterococcus species | Chronic wounds and hospital-acquired infections |
| Anaerobic bacteria | Deep ulcers, often in combination with others |
| Fungi | Rare, more likely in immunocompromised |
Staphylococcus aureus (including MRSA), often just called “staph,” is particularly adept at evading immune defenses and forming protective biofilms on bone or within dead tissue. Other organisms include Pseudomonas aeruginosa, and other gram-negative bacteria. When a wound stays open or untreated, these bacteria seize the opportunity.
In rare cases, fungi or other less common bugs may be found, especially in people with weakened immune systems, but bacteria remain the primary cause.
Signs and Symptoms to Watch For
Foot osteomyelitis rarely presents with a single unmistakable symptom. Instead, it can mimic more benign problems, making it easy to misinterpret or initially miss. Classic signs, where present, may include:
- Persistent pain in the affected foot, sometimes worsened by movement or touch
- Redness, warmth, and swelling localized over the infected area
- A non-healing ulcer, particularly one that exposes bone or does not improve with standard wound care
- Foul-smelling drainage from a wound or sinus tract
- Fever or chills (more often in acute cases)
- Fatigue or general malaise
- Difficulty bearing weight or walking
A helpful tip: Any wound near a bone that can be probed with a sterile instrument and touches bone underneath is highly suspicious for underlying osteomyelitis.
The story can be different for people with neuropathy, who might not feel pain. Here, a sore that lingers, continues to drain, or shows exposed bone should raise alarm, even in the absence of classic infection signs. If you have diabetes and notice a wound that isn’t healing, it’s crucial to seek medical evaluation promptly from Dr. Hoy.
Chronic vs. Acute Osteomyelitis
The timeline and context can give important clues.
- Acute osteomyelitis develops within two weeks of the initial infection or injury. It typically causes marked pain, redness, possibly fever, and general symptoms.
- Chronic osteomyelitis can smolder for months or years. The pain may come and go, and wounds may intermittently heal, only to open again. Bone damage, dead bone (sequestrum), and persistent drainage often result.
Chronic forms are more challenging to cure, especially when healing is impaired.
Diagnosing Foot Osteomyelitis
Accurate diagnosis is essential for effective treatment. Common diagnostic methods include:
- Medical history and risk assessment
- Physical exam, looking for wounds, swelling, signs of infection, probing the wound, and exposed bone
- Blood tests, including inflammatory markers (elevated white blood cells, C-reactive protein, ESR), though these may be bland in chronic cases
- Imaging studies:
- Plain X-rays May show bone erosion (can miss early infections—changes often seen after 2–3 weeks)
- MRI scans (the most sensitive for early detection, especially valuable in diabetic foot)
- CT scans Useful in complex cases (helpful for planning surgery or assessing bone destruction)
- Bone biopsy and culture: This is the gold standard, allowing precise identification of the infecting organism and determining which antibiotics will work best.
Non-healing ulcers overlying bone, or those that fail to respond to ordinary wound care, frequently prompt a search for hidden osteomyelitis.
Treatment Options for Foot Osteomyelitis
Our Seattle office provides both antibiotic and surgical treatment for foot osteomyelitis. Treatment depends on the severity and chronicity of the infection:
1. Antibiotics
- Usually started intravenously (IV) and may continue orally for weeks.
- Targeted based on culture and sensitivity results.
2. Surgical Debridement
- Removal of infected or necrotic bone tissue.
- May involve minor or extensive procedures, depending on the spread.
3. Wound Care
- Specialized foot care to promote healing.
- Use of negative pressure wound therapy or advanced dressings.
4. Hyperbaric Oxygen Therapy (HBOT)
- Occasionally used to improve oxygenation and aid healing in chronic infections.
5. Amputation
- In severe cases where the infection is uncontrolled or limb-threatening.
Why Early Recognition Matters
If you experience persistent foot pain, notice signs of infection, or have a non-healing ulcer—especially with underlying conditions like diabetes—consult a healthcare provider immediately. Early diagnosis and treatment of foot osteomyelitis can prevent serious complications.
Delay in identifying and treating foot osteomyelitis can have severe consequences:
- Loss of bone integrity, leading to deformity or fractures
- Spread of infection to joints, soft tissue, or the bloodstream (sepsis)
- Poor wound healing and ongoing pain
- Higher risk of amputation
Early intervention often means less aggressive surgery or a shorter course of antibiotics, with better chance of preserving foot structure and mobility.
Key Points for Patients and Providers
A few reminders can help both patients and healthcare professionals stay alert:
- Don’t ignore chronic wounds: Especially in those with diabetes or vascular disease.
- Pain is not always present: Absence of pain does not rule out infection, particularly in those with neuropathy.
- Ask about sensation: People with neuropathy may not notice new injuries.
- Look for “probe to bone”: If you can touch bone in an ulcer, suspicion should be high.
- Imaging matters: Advanced scans pick up what plain X-rays might miss.
- Act quickly: The sooner treatment begins, the better the outlook.
Preventive Strategies
For those at risk, a few strategies make a big difference in preventing foot osteomyelitis:
- Meticulous foot hygiene and daily inspection
- Properly fitting footwear to avoid blisters and pressure sores
- Regular visits with a podiatrist like Dr. Hoy for those with diabetes
- Early, aggressive care for even minor wounds
- Tight control of blood sugar and addressing vascular risk factors
Foot osteomyelitis is a complex but treatable condition. With timely medical intervention, most patients can recover without long-term damage. Understanding the signs, risk factors, and treatment options is key to effective management and prevention.
