A neuroma is like a tangled garden hose causing water flow disruption.
Just as a kinked hose may prevent water from reaching a distant plant, a neuroma, particularly Morton’s neuroma, can disrupt the normal communication pathways between nerves and feet, causing discomfort. While often benign, addressing the symptoms early can prevent further complications and ensure our nervous “gardens” flourish and thrive without interruption. With understanding and timely intervention, we possess the power to untangle these nerve endings, ushering in continued wellness and vitality.
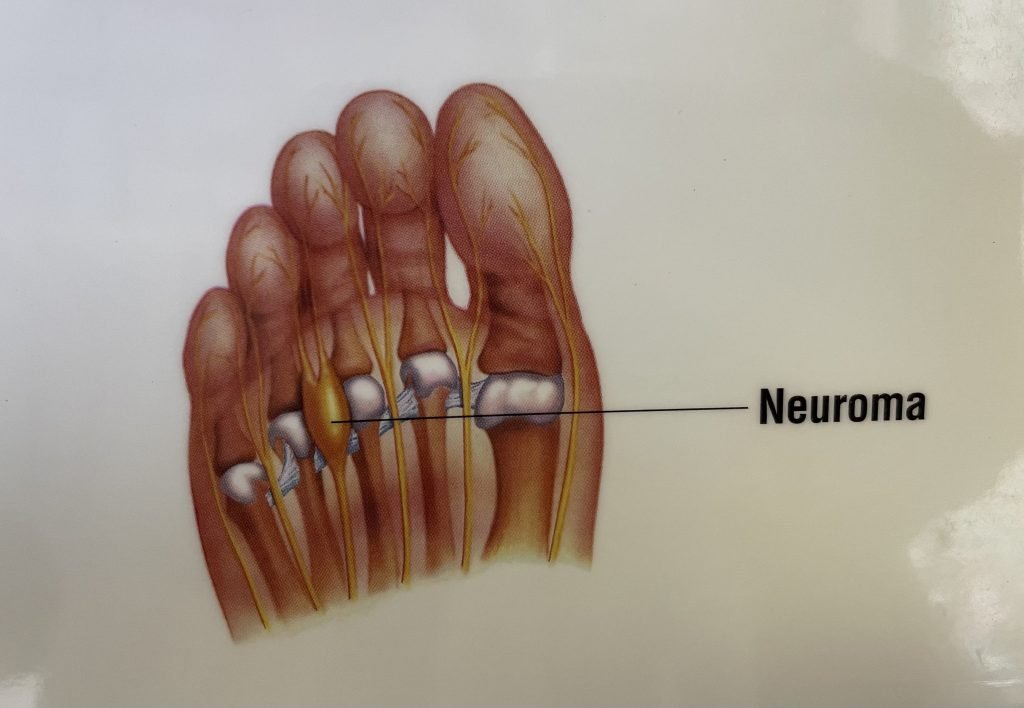
What is a Neuroma?
A neuroma is a benign growth of nerve tissue that can manifest as a painful sensation in the body.
Typically, these nerve growths occur in the foot, particularly between the toes, causing symptoms such as sharp, burning pain, tingling, or a feeling of a pebble in the shoe. Morton’s neuroma is a common type associated with nerve enlargement between the third and fourth toes, often influencing everyday comfort and mobility.
Interestingly, this condition is not a true tumor but rather a thickening of nerve tissue. As compression and irritation, often from ill-fitting footwear or repetitive activities, increase, the affected nerve enlarges, becoming more sensitive and painful.
With early diagnosis and appropriate management, many individuals successfully alleviate symptoms, resuming their active lifestyles with ease. Treatments range from modifications in footwear to advanced medical interventions that target the nerve’s distress. This knowledge empowers both prevention and rehabilitation, transforming neuroma management into an opportunity for revitalized well-being.
Common Types of Neuroma
Neuromas, despite being commonly associated with the foot, can manifest in various locations throughout the body. Each type has specific characteristics that contribute to its distinction among other nerve-related conditions.
Morton’s neuroma is the most prevalent type, typically occurring between the third and fourth toes. This condition results from compression and irritation, often exacerbated by footwear choices that apply undue pressure to the forefoot. Prompt intervention can mitigate discomfort and restore mobility effectively.
Acoustic neuroma, also known as vestibular schwannoma, is another noteworthy type that affects the nerves responsible for hearing and balance. Although benign, it can lead to significant symptoms such as hearing loss and dizziness if left untreated, often necessitating careful monitoring or surgical intervention.
Further, other forms such as traumatic neuroma arise from nerve injuries and may occur after surgeries or accidents. Such neuromas highlight the body’s intricate healing processes, where nerve ends attempt to repair themselves, yet end up forming these benign proliferations.
Understanding these variations enhances our ability to address neuroma comprehensively, ensuring each individual receives tailored care. Empowered with this knowledge, we continue to advance towards a future where pain from neuromas is efficiently alleviated.
Causes of Neuroma
Neuromas primarily evolve from repetitive mechanical stress.
This stress often arises from high-pressure activities. The most common neuroma, Morton’s neuroma, frequently results from excessive compression of nerve tissue in the forefoot, typically exacerbated by ill-fitting shoes or high heels. Additionally, engaging in sports that require significant use of the feet, such as running, can also contribute to the development of this condition.
Congenital anomalies may influence neuroma formation.
Pre-existing foot deformities or abnormalities naturally increase susceptibility – an inherent arch issue or chronic alignment imbalance can lead to intensified nerve compression, thus heightening neuroma risk. Furthermore, inflammatory conditions such as arthritis can exacerbate these predispositions.
Understanding these causes of neuroma not only illuminates potential preventive strategies but also inspires hope. By blending cutting-edge research and innovative treatment approaches, healthcare professionals can develop more personalized solutions to combat neuroma. Together, we harness this evolving knowledge to transform lives, empowering individuals to step confidently into a future free from neuroma discomfort.
Risk Factors Associated with Neuroma
Certain occupations and activities elevate neuroma risk.
Prolonged standing or walking on hard surfaces is a significant factor. Jobs that demand long hours on the feet, such as retail or food service, significantly contribute to increased neuroma incidences. Additionally, professions that necessitate restrictive footwear, such as fashion or dance, amplify this risk exponentially.
Age also plays a pivotal role.
As individuals age, the protective layer of fat pads under the toes can thin, placing extra stress on nerves. This naturally occurring change becomes particularly important in neuroma contexts, where added pressure accentuates the likelihood of nerve irritation.
The interplay of genetics cannot be overlooked, emphasizing the need for vigilance. Family history holds significant sway, providing valuable genetic clues to predisposition. Through awareness and proactive action, we can curb the impact of these hereditary tendencies, charting a promising course toward a healthier, neuroma-free future.
Recognizing Neuroma Symptoms
Recognizing neuroma symptoms early is important for effectively managing the condition. People often report sharp, burning pain or tingling sensations in the balls of their feet, usually between the third and fourth toes. As it progresses, the discomfort can become persistent, creating challenges in everyday activities and impacting quality of life.
The term “Morton’s neuroma” or “interdigital neuroma” commonly describes this type of nerve compression.
Physical Symptoms
Individuals experiencing a neuroma often notice a sensation of fullness or a burning ache, which escalates while walking. Pain typically surfaces in the forefoot region, disrupting natural movement.
Symptoms may also include numbness or tingling, which patients frequently describe as a “pebble” feeling underfoot. Throbbing, while rare, can be a sign of irritated nerves struggling to function correctly.
Ignoring neuroma symptoms can lead to further nerve damage, emphasizing the importance of early diagnosis and treatment.
Repeated activity without intervention leads to exacerbation, presenting challenges in maintaining active lifestyles. Proper footwear and early medical consultation can greatly aid symptom management, setting a proactive pathway to alleviate discomfort and regain mobility. Embracing these measures can remarkably enrich one’s well-being, underscoring the power of informed health choices.
Neurological Impact
Neuromas, though often localized, can have significant neurological effects on both physical and mental wellness.
When a neuroma develops, its perturbation of the nerve tissue generates an altered signaling pattern, causing discomfort. The continued pressure and irritation induce miscommunication within the nervous system, affecting not just the site of the neuroma, but also potentially causing referred pain or dysfunction throughout the body.
Remarkably, the presence of a neuroma sparks a cascade of responses within the nervous system. As individuals adapt to ongoing discomfort, they may unconsciously alter their gait, inadvertently leading to secondary issues in posture and muscle strain, exacerbating the initial neurological disruption.
Recognizing the neurological impact of a neuroma is critical in crafting a comprehensive approach to treatment. By addressing both the direct symptoms and the resulting neurological adaptations, healthcare providers can effectively tailor holistic strategies. This proactive method not only alleviates immediate pain but also empowers individuals to reclaim strength and embrace vibrant health, illustrating the profound possibilities of strategic intervention and rehabilitation.
How is Neuroma Diagnosed?
Diagnosing a neuroma involves a meticulous evaluation of the patient’s medical history, detailed examination, and clinical tests. Physicians first assess symptoms, such as pain, tingling, or numbness.
In addition, they employ imaging studies to gain deeper insights. Techniques like ultrasound provide detailed views, aiding surgeons in assessing and planning further treatment.
Diagnostic tools, such as magnetic resonance imaging (MRI) and electromyography (EMG), are essential for diagnosing neuromas. These tools empower physicians to distinguish neuromas from other conditions, ensuring accurate and tailored therapeutic strategies.
Ultimately, the journey to a precise neuroma diagnosis is one of collaboration and expertise. Encouraging patients to openly share their experiences with healthcare providers is pivotal, as it leads to a customized care plan addressing unique needs. In this way, diagnosis can be a transformative step toward reclaiming vitality and well-being.
Medical Imaging Techniques
Within the realm of neuroma diagnosis, medical imaging techniques stand as powerful tools, illuminating the often hidden intricacies beneath the skin’s surface. By leveraging cutting-edge technology, healthcare professionals can gain unparalleled insights into the structure and behavior of neuromas.
Among these techniques, MRI is particularly valuable for diagnosing neuromas. It reveals soft tissue structures with remarkable clarity and precision.
Furthermore, ultrasound imaging is increasingly relied upon due to its ability to provide real-time visualization of neuromas. It aids in assessing the character and exact location of these growths.
Medical professionals may also utilize computed tomography (CT) scans as part of their diagnostic toolkit. These scans deliver detailed cross-sectional images, enhancing the capacity to detect and evaluate neuromas with confidence.
Together, these advanced imaging modalities enable a comprehensive assessment of neuromas, guiding effective treatment plans. As healthcare teams integrate these technologies, they chart a path toward improved patient outcomes and fulfilled health journeys.
Indeed, the application of these sophisticated imaging techniques brings the prospect of targeted and successful treatment within reach. They exemplify the extraordinary synergy between technology and medicine, crafting a promising future for individuals living with neuromas.
Treatment Options for Neuroma
When addressing neuromas, numerous treatment paths are available to enhance patients’ well-being and comfort. Depending on severity, healthcare practitioners may recommend conservative therapies such as orthotics or anti-inflammatory medications, which aim to reduce symptoms and manage discomfort effectively. For cases requiring more direct intervention, options include corticosteroid injections or surgery, each serving to eliminate pain and restore patients’ active lifestyles.
Ultimately, whether one opts for conservative management or surgical solutions, the overarching goal remains consistent—enabling individuals to return to their daily activities without hindrance from neuroma-induced pain.
Non-Surgical Approaches
In the pursuit of alleviating neuroma symptoms, non-surgical methods offer promising and effective alternatives for many individuals seeking relief.
Custom orthotics stand out as powerful tools in the arsenal against neuromas. They focus on adjusting biomechanics, thereby reducing nerve pressure and associated discomfort. Through these personalized interventions, patients often experience significant improvement in their condition without recourse to surgical procedures.
Furthermore, embracing lifestyle modifications can play a crucial role in managing symptoms. Alterations to footwear, incorporating cushioned insoles, and avoiding activities that exacerbate the condition serve as simple yet transformative strategies. These changes foster an environment of healing, promoting comfort and functionality in everyday life.
Evidence-based practices, such as physical therapy, massage therapy and ultrasound therapy, have been shown to alleviate neuroma-related pain. By enhancing circulation and reducing inflammation, these therapies complement other treatments, presenting a multi-faceted approach that empowers patients on their path to recovery.
Ultimately, the panoramic vista of non-surgical approaches illuminates a hopeful pathway to regaining a joyful, active lifestyle while minimizing the disruptions posed by neuroma.
Surgical Interventions
Surgical interventions for neuroma offer a targeted approach when conservative treatments do not sufficiently alleviate symptoms, paving the way for restored comfort and functionality.
- Neurectomy: Involves removing the affected nerve to eliminate pain directly.
- Decompression Surgery: Aims to relieve pressure on the nerve by cutting surrounding ligaments.
- Sclerosing Alcohol Injections: Used as a minimally invasive alternative to surgery, achieving pain relief by destroying nerve tissue.
- Radiofrequency Ablation: Involves using heat to disrupt nerve function, providing significant pain reduction.
These surgical procedures are designed to offer lasting relief for patients suffering from severe neuroma symptoms.
Careful consideration and consultation with medical professionals can ensure that the most appropriate surgical option is chosen, tailored to individual patient needs.
Preventing Neuroma Development
Elevate your foot health with proactive choices today.
Preventing neuroma development begins with proper footwear. The simple act of choosing shoes that offer adequate support and are the right size can be instrumental in maintaining foot health. Moreover, opting for styles that ensure spacious room for toes significantly reduces the risk of nerve compression. Regularly, assessing the fit of your shoes helps in mitigating the discomforts associated with tight footwear.
Incorporate foot exercises into your daily routine.
These exercises focus on strengthening foot muscles, improving circulation, and aiding in flexibility, all of which collectively diminish the chance of neuromas. Additionally, staying vigilant about maintaining a healthy weight can alleviate unnecessary pressure on your feet, further diminishing potential strain on the nerves.
Empower yourself with knowledge by consulting healthcare professionals who specialize in orthopedics or podiatry, like Dr. Hoy, especially if foot discomfort arises. Being proactive in managing foot health with consistent check-ups can lead to early detection, offering the best chance to utilize preventive strategies effectively and enjoy enduring comfort and mobility.
When to Seek Medical Advice
Understanding when to reach out for medical advice is paramount in addressing neuroma symptoms effectively. Proper intervention at the right moment can dramatically improve outcomes. Our Seattle office is experienced in treating neuromas.
Seek medical attention promptly if you notice persistent foot pain. Persistent aches should not be ignored.
Notably, changes such as a sensation of burning, tingling, or numbness warrant immediate consultation. These symptoms may indicate critical nerve involvement.
Additionally, experience of sharp pains, especially those that intensify with pressure or while wearing shoes, calls for professional evaluation. An early diagnosis enables more effective management.
Furthermore, if rest and conservative treatments fail to provide relief, consulting a healthcare provider could open a pathway to alternative solutions. Exploration of treatments such as orthotic devices or physical therapy could be necessary.
Remember, you are not alone in navigating what’s happening with your feet. Proactive medical intervention ensures that you reclaim comfort and function, geared towards a more active and fulfilling life.
Living with Neuroma Management Strategies
Navigating neuroma necessitates informed strategic action.
To enhance quality of life with neuroma, start with creating a robust support team of healthcare professionals who understand your unique situation. These experts may guide you towards potential treatment plans, such as custom orthotics, physical therapy, and activity adjustments. Decades of research validate collaborating with trusted medical advisors fosters improved outcomes.
Empower yourself with knowledge.
Adopting an iterative approach to treatment empowers patients. This means continually reassessing and adapting strategies based on response to interventions—be it through innovative pharmaceutical options, next-level therapies, or lifestyle adjustments. Flexibility in treatment enhances adaptability, promotes healing, and paves the way for sustained comfort.
Incorporating holistic approaches such as stress management, healthy eating, and regular exercise contributes to comprehensive care. Engaging in activities that foster both physical and emotional wellness ensures a holistic recovery journey, reducing neuroma impact significantly. Strive for resilience and be patient; your efforts will yield transformative progress.
“Dr. Hoy is experienced, knowledgeable, and personable. I developed Morton’s Neuroma and I’ve learned so much about treating it, what to do to relieve/minimize the pain, I received proper treatment, and learned what foot attire to wear for comfort. The office manager, Jessica, is absolutely wonderful, too. Highly recommend Dr. Hoy! Complete confidence in him.” -Lalanie C.
